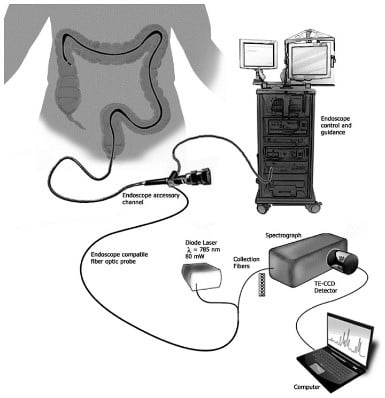
Researchers have developed the first sensor capable of objectively identifying inflammatory bowel disease (IBD) and distinguishing between its two subtypes. The device marks an important development toward a more personalized approach to diagnosing IBD, a chronic inflammation of the gastrointestinal tract affecting more than 1 million Americans.
Developed as a minimally invasive probe that can be integrated easily into a routine colonoscopy exam, the sensor could help physicians to diagnose IBD and evaluate a patient’s response to treatment, claim its developers at Vanderbilt University.
Current diagnostic and treatment procedures are inexact and largely rely on trial-and-error. A diagnosis typically depends on how the patient responds to therapy over time. Often, a few years may pass before a definitive diagnosis can be made.
Anita Mahadevan-Jansen, director of the Biophotonics Center at Vanderbilt University and a senior author of the paper, says, “That’s why we decided to use a light-based method to probe the biochemistry of what’s going on in the colon. Our goal is to use Raman spectroscopy to look at the actual inflammatory signals.”
SEEKING A GOLD STANDARD FOR DIAGNOSIS
Currently, a combination of clinical, radiologic and pathological methods are used to diagnose a patient’s IBD subtype and guide treatment decisions. But these methods detect symptoms instead of the underlying source of the disease. As a result, up to 15% of patients are diagnosed with indeterminate colitis, meaning the subtype is unknown, and an additional 5% to 14% have their IBD reclassified based on how they respond to treatment.
IBD occurs in two subtypes: ulcerative colitis (UC), which is typically confined to the colon, and Crohn's disease, which can occur in any part of the
gastrointestinal tract,
reports Phys.org. Both can cause similar symptoms such as severe diarrhea, pain, fatigue and weight loss, but the two types respond differently to available treatments.
Previous research conducted on tissue samples from people with IBD showed that UC and Crohn's disease model different molecular signature. The new probe detects these signatures in order to glean information about not only disease subtype, but also the current degree of inflammation and even early indicators of IBD that occur before observable changes in the intestinal tissue.
“Most people go through baseline colonoscopy as part of routine care, and you could imagine using this to get a baseline Raman signal for each person,” Mahadevan-Jansen says. “If someone presents with IBD symptoms later on, you can use our system again to determine if it’s more likely to be UC or Crohn’s. Then once they are being treated, you have an objective measure to track their response because you can use the device to actually quantify mild, moderate or severe inflammation.”
LOOKING AHEAD
The researchers are now focused on refining a set of algorithms that help doctors interpret test results for a given patient. To improve the specificity of the test, the team is analyzing data from an expanded cohort of patients to discern how factors such as gender, diet, demographics and treatment regimen influence the Raman signature.
Ultimately, the researchers envision a system that combines key information about the patient with Raman spectra to deliver, in a matter of seconds, tailored results that can inform a diagnosis or help track a patient’s response to treatment.
“It’s a unique way of thinking about personalized medicine that takes into account all sorts of information beyond just the genome, including demographics and many other factors that make a person unique,” notes Mahadevan-Jansen. “Our lab has really pushed to find ways to apply optical technology to support this kind of personalized medicine.”
The study signals the huge potential of Raman spectroscopy in the field of medical diagnostics.
According to BCC Research, the market for medical diagnostics should almost double in value from 2016-2021, thanks to a hefty compound annual growth rate. Overall, the global market for Raman spectroscopy is expected to reach $1.8 billion by 2021 from $1.1 billion in 2016, growing at a CAGR of 9.9% from 2016 through 2021.