Sep 19, 2016
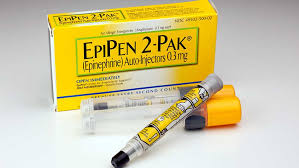
Blog Life Sciences Mylan’s EpiPen is Just the Latest Contributor to Drug-Pricing Debate
There’s a constant grumbling in the background when it comes to the prices of pharmaceuticals. Treatments for oncology and the hepatitis C virus are widely cited as among the most expensive medications. So, too, are certain therapies for orphan indications. The latest example to evoke widespread criticism is that of Mylan NV’s EpiPen device for treatment of severe allergic reactions. The EpiPen’s price has soared more than 400% since Mylan acquired the product in 2007, to more than $600 now, sparking outrage from patients, consumers, and politicians.
But without strong competitors, Mylan’s EpiPen still holds an estimated 94% market share in the United States. Now, Teva Pharmaceutical Industries Ltd. has stepped forward to say that it aims to win US approval by late 2017 or early 2018 for its version of Mylan’s EpiPen. Teva’s application for a copycat version has been in question since February, when the FDA flagged “major deficiencies” in the generic company’s device. Amid the growing controversy, Mylan has said that it will launch its own $300 generic version of the EpiPen.
The story is an old one with a recurring theme. Other high-profile cases of so-called price gouging in more recent history include those of Valeant Pharmaceuticals International Inc. and of Turing Pharmaceuticals. In February 2015, Valeant bought the rights to two life-saving heart drugs, Nitropress and Isuprel. It raised the list price for Nitropress by 525% and for Isuprel by 212%, leading to a congressional investigation. Six months later, these flames were fanned by Martin Shkreli, CEO of Turing Pharmaceuticals at the time, who, upon acquiring an older drug called Daraprim, hiked its price by a staggering 5,000% overnight.
In addition to the heart drugs, in early October of 2015 a Deutsche Bank analysis concluded that Valeant had jacked up prices on 54 other medicines in 2015 alone, by an industry-leading average of 65.6%. (In 2014, Valeant hiked the prices on 62 drugs by an average of 50%.) Shortly thereafter, Valeant received a federal subpoena over its drug-pricing strategy. Days later, on an earnings call with analysts, Valeant CEO J. Michael Pearson said that the company was backing down from its long-running strategy of buying older drugs and raising the prices.
In July 2015, the FDA approved the drugs Praluent (Sanofi US and Regeneron Pharmaceuticals, Inc.) and Repatha (Amgen, Inc.) as the first in a new class of cholesterol drugs called PCSK9 inhibitors. These agents can reduce heart attack–causing cholesterol by up to 60%, but are priced at $14,000 per year. These drugs treat a common condition and need to be taken for the rest of a patient’s life. Giving the drugs to all 9 million eligible patients in the United States could increase the nation’s total health costs by $120 billion, according to an analysis in JAMA.
As mentioned above, in August 2015, Turing Pharmaceuticals hiked the price of Daraprim, a drug that treats dangerous infections in people who are weakened by AIDS and cancer, from $13.50 to $750 per pill. Shkreli was famously blackballed, resigned as CEO of Turing, and was arrested by the FBI after being indicted on federal charges of securities fraud. Now, one pill of Daraprim costs $375 for many patients, which is still 2,500% more than before the hike. Before 2010, Daraprim only cost $1.
In many cases, it is asserted by drug makers that the at times eye-popping prices are justified by the high investments made in the research and development of the therapeutic. It’s a heated, complicated debate being grappled with by drug makers, politicians, patients, payers, and physicians. Earlier this year, the Pharmaceutical Research and Manufacturers of America (PhRMA) launched a campaign it calls “From Hope to Cures” to highlight the value that biopharmaceutical innovation provides to patients, society, and the economy. On its Web site, it states that PhRMA member companies invested $58.8 billion in research and development in 2015.
And, drug prices may be expensive, but they cost a whole lot less than the alternative, says the Biotechnology Innovation Organization (BIO), in its latest marketing campaign. This week, BIO launched its new ad campaign, which is strikingly similar to PhRMA’s, called “Innovation Saves,” to highlight the value of biopharmaceutical innovation. The group is planning to spend between $1 million and $5 million on the campaign, which will include television ads and a web resource.
With such a tangled web of players, there is one thing that seems clear. Any future “win–win” solution will be extraordinarily hard won.

Here's the problem: biology is generating data faster than anyone can analyze it...
In today’s fast-paced biomedical world, researchers and pharmaceutical companies...
Radiopharmaceuticals represent a cutting-edge frontier in modern medicine, offer...

We are your trusted research partner, providing actionable insights and custom consulting across life sciences, advanced materials, and technology. Allow BCC Research to nurture your smartest business decisions today, tomorrow, and beyond.
Contact UsBCC Research provides objective, unbiased measurement and assessment of market opportunities with detailed market research reports. Our experienced industry analysts assess growth opportunities, market sizing, technologies, applications, supply chains and companies with the singular goal of helping you make informed business decisions, free of noise and hype.